INSURANCE COVERAGE RESOURCES
There are significant changes in Medicaid coverage that are taking place. Don’t lose your health insurance coverage. Contact a Financial Navigator to help you with this process today.
“Windrose Health Network will not deny services to anyone based on an inability to pay.”
“Windrose Health Network no negará a servicios a nadie que por no poder pagar.”
“Windrose Health Network nih a man liam khawh lo ruang ah mi zei hmanh service pek lo in a um lai lo.”
-------------------------------------------------------------------------------------------------------------------------------------------------------------------------------
“Windrose Health Network has a discounted/sliding fee schedule available based on family size and income.”
“Windrose Health Network tiene una tarifa de descuento disponible según el tamaño de la familia y los ingresos.”
“Windrose Health Network nih income le chungkhar milu tuak in a man thumh piak khawhnak Sliding Fee Schedule timi a ngei."
Our Navigators
WindRose Health Network offers complimentary Enrollment Services to assist our communities with enrollment into various health coverage programs such as Hoosier Healthwise, Healthy Indiana Plan (HIP), Marketplace Insurance and Medicare assistance. Please contact the enrollment Eligibility Navigator nearest you to schedule an appointment. You can click on their name below for contact information.

Vernlal Englian, CAC, CIN, CHW, SHIP
EPLER PARKE

Grecia Gonzales Flores, CIN, CAC, CHW, SHIP
FRANKLIN CENTER

Biak Mawi, CIN, CAC, SHIP
EPLER PARKE

Rebecca Moore
Trafalgar Center

Jo Turnbloom, CIN, CAC, SHIP, LCHW
FRANKLIN CENTER

Kara Fields, CIN, CAC, SHIP
Eligibility Navigator

Lily Hoi
SHIP Counselor, Eligibility Navigator
Programs and Services

Hoosier Healthwise (Medicaid)
In order for you to become eligible for Hoosier Healthwise, you must first complete an application. Click and complete a request to connect with an Eligibility Navigator.
REQUEST AN APPOINTMENT
Healthy Indiana Plan (HIP)
The Healthy Indiana Plan covers Indiana residents between the ages of 19 and 64 whose family incomes are less than approximately 138 percent of the federal poverty level and who are not eligible for Medicare or another Medicaid category. Click and complete a request to connect with an Eligibility Navigator.
REQUEST AN APPOINTMENT

New to Medicare
Wether you are transitioning from HIP to Medicare or are or new to Medicare, we can help you get signed up. Medicare is the country’s health insurance program for people age 65 or older. Certain individuals under the age of 65, including those with disabilities and those who have end-stage renal disease (ESRD), can qualify. This program helps with the cost of health care and has additional extra help plans that could assist you with specific premiums and additional costs. Click and complete a request to connect with an Eligibility Navigator.
REQUEST AN APPOINTMENT

Marketplace
Marketplace Plans offer the ability to compare and enroll into various offered plans. Plans include no annual or lifetime dollar limits for essential health benefits. Dental and vision coverage can be purchased along with Health Plan. Click and complete a request to connect with an Eligibility Navigator.
REQUEST AN APPOINTMENT

FindHelp.org
Findhelp.com allows you to search by zip code and connect to a variety of free and reduced-cost programs and services. Our patients can use findhelp.com technology to support their social care needs across 10 dimensions of care including food, housing, goods, transit, health, money, care, education, work and legal.
LEARN MORE

Your Insurance Questions Answered
The Indiana Primary Health Care Association, which advocates for quality health care for all persons residing in Indiana, provides information and videos about the most frequent questions about the health insurance marketplace.
Learn more
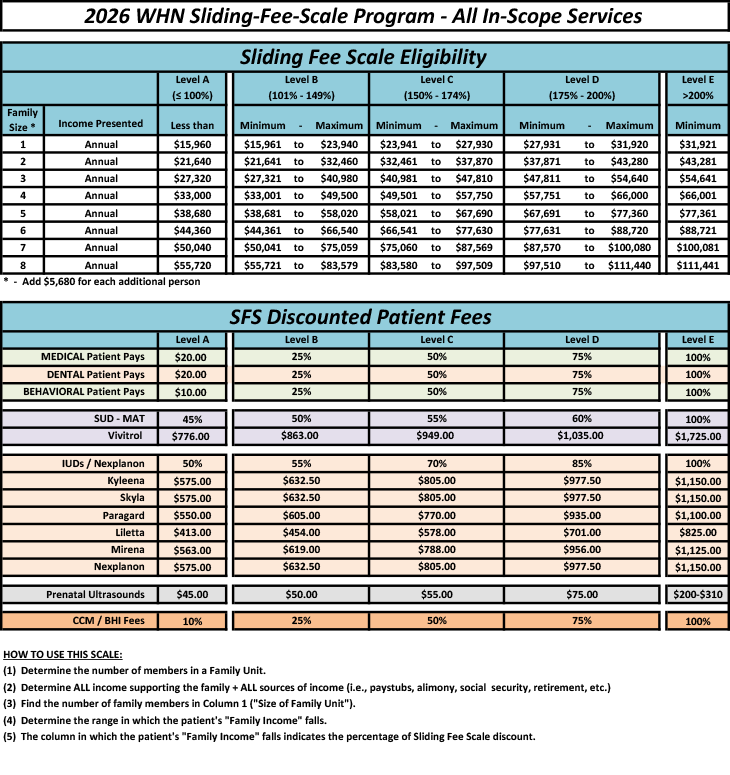
Sliding Fee Discount
If you or any members of your family meet the eligibility requirements, you may qualify for reduced-cost health services through our Sliding Fee Scale. To see if you are eligible for discount services, please use the annual income guidelines on this chart.
In order to become eligible for the WHN ’s Sliding Fee Discount Program, you must first complete a Sliding Fee Scale application. We encourage you to contact an Eligibility Navigator listed above at a location nearest to you. For your security, please do not submit SFS documents through the website. Call your health center to schedule an appointment with a Financial Counselor to complete the application process.
How to Use The Sliding Fee Scale
Determine the number of household members claimed on your Federal Income Taxes.
- Determine the yearly income of ALL household members 19 and older. Sources of income (i.e., pay stubs, employer statement, Tax Return, Social Security, etc.)
- Find the total number of household members claimed on the patient’s federal taxes in Column 1 ("Size of Family Unit").
- Determine the range in which the patient's "Household Income" falls.
- The column in which the patient's "Household Income" falls indicates the percentage of Sliding Fee Scale discount.
Federal Poverty Guidelines
The Federal Poverty Guidelines are federally set “poverty lines” that indicate the minimum amount of annual income that an individual/family needs to pay for essentials, such as housing, utilities, clothing, food and transportation. These guidelines, also called Federal Poverty Levels (FPLs), are based on the size of a household and the state in which one resides.
Good Faith Estimate
You have the right to receive a “Good Faith Estimate” explaining how much your medical care will cost
Under state and federal law, a patient who doesn’t have insurance or who is not using insurance may ask a health care provider for a Good Faith Estimate (“GFE”). The GFE is the price the health care provider and health facility will charge for providing non-emergency health care services, In addition:
- You have the right to receive a Good Faith Estimate for the total expected cost of any non-emergency items or services. This includes related costs like medical tests, prescription drugs, equipment and hospital fees.
- Make sure your health care provider gives you a Good Faith Estimate in writing at least one business day before your medical service or item. You can also ask your health care provider and any other provider you choose for a Good Faith Estimate before you schedule an item or service.
- Patients who are uninsured or self-pay may dispute the actual charges if the actual charges exceed the Good Faith Estimate by at least $400.
- Make sure to save a copy or picture of your Good Faith Estimate.
call 317.680.9093
Email UsFor questions or more information about your right to a Good Faith Estimate, click here or call 800.985.3059.

Medication Assistance
Adult patients may apply for free or reduced-cost medications through the Assisted Medication Program (AMP). To apply you will need to share proof of household income with each application. Examples of documents are:
- Prior year tax return
- Paycheck stubs from the past 30 days
- Social Security Office Award Letter
If approved, your medication(s) should arrive within six to eight weeks. It is your responsibility to call your provider and request a refill four weeks in advance of your current medication running out.
WHN cannot guarantee that you will meet the drug company’s rules or that your medication(s) are available through AMP. Please note: It is the strict policy of WHN not to allow narcotic medications to be ordered through AMP.